
Diagnosis of Cystic Acne
Physical Examination
Diagnosis of cystic acne typically involves a thorough physical examination by a qualified healthcare provider. In some instances, microbiological tests may be conducted, especially if gram-negative bacteria are suspected to be involved. Endocrinology tests can also be performed to assess any hormonal imbalances that may be contributing to the condition.
Acne varies in severity, manifesting as mild, moderate, or severe forms. Commonly, the affected areas include the face, back, and chest. A typical acne presentation features a mix of open and closed comedones—commonly known as blackheads and whiteheads—as well as inflammatory lesions like papules and pustules. Additional symptoms may include scarring, excessive sebum production, and post-inflammatory pigmentation.
It’s worth noting that pilosebaceous units, the skin structures involved in acne, are present almost everywhere on the body except for the palms, soles, and certain areas of the lips and feet. These units are most densely populated on the face, chest, and upper neck, which explains why acne is most frequently observed in these regions.
Microbiological Testing For Acne
Microbiological tests are often used to identify the specific bacteria contributing to acne. Typically, the bacteria involved are gram-positive and naturally occur on the skin. However, in certain instances, gram-negative folliculitis may be present. This condition is characterized by pustules and nodules, primarily located around the mouth and nose areas.
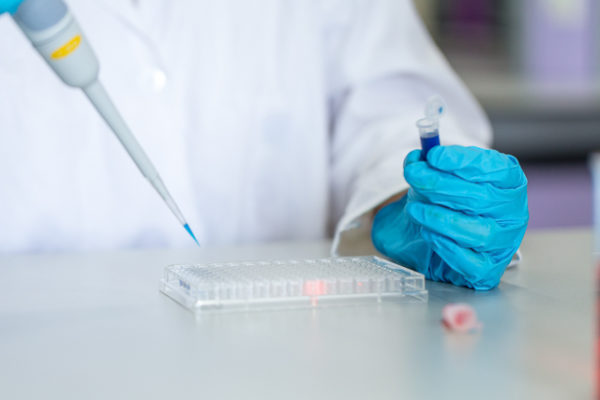
The skin microbiome is a complex ecosystem that includes a variety of microorganisms, such as bacteria, viruses, and fungi. Among these, Propionibacterium acnes and Malassezia spp. have been implicated in the development of acne by influencing sebum secretion, comedone formation, and the inflammatory response. Therefore, understanding the microbiome’s role in acne can offer valuable insights into its management and treatment.
In summary, while microbiological testing is not always a standard procedure in the diagnosis of acne, it can be particularly useful in cases where standard treatments have failed or where there is suspicion of atypical bacterial involvement.
Endocrinological Evaluation for Acne
Based on information from multiple sources, endocrinological tests are not typically the first line of investigation in diagnosing acne. However, they can be an essential part of a comprehensive diagnostic approach, especially for women with persistent or severe acne. These tests aim to assess hormonal imbalances that may contribute to acne, such as elevated levels of androgens or imbalances in estrogen and progesterone.
A study published on PubMed emphasizes the importance of endocrinological evaluation and hormonal therapy for women with difficult-to-treat acne.
A dermatologist should be consulted if over-the-counter acne products have not been effective, as more specialized tests like endocrinological evaluations may be necessary in such cases.
In summary, while endocrinological tests are not usually the initial step in acne diagnosis, they can provide valuable insights into underlying hormonal imbalances that may be exacerbating the condition. These tests are particularly useful for women with severe or persistent acne and can guide more targeted treatment options.
Conditions Mistaken For Cystic Acne
It is important to recognize that acne outbreaks can present with a variety of lesions, including comedones, papules, pustules, nodules, and different types of scarring. When patients don’t respond well to standard acne treatments, despite following the prescribed regimen diligently, it may be due to a misdiagnosis. Several conditions can mimic the symptoms of acne, leading to ineffective treatment and prolonged suffering.
Conditions that are commonly mistaken for acne include Folliculitis, which is an inflammation of the hair follicles, and Miliaria, also known as heat rash. Syringoma, a benign tumor of the sweat glands, and Sebaceous Hyperplasia, an enlargement of the sebaceous glands, can also be confused with acne. In some instances, skin infections caused by Staphylococcus aureus bacteria, including Methicillin-resistant Staphylococcus aureus (MRSA), can present with large, painful bumps that closely resemble acne lesions.
Moreover, conditions like rosacea can be triggered by environmental factors such as sun, heat, and humidity, leading to flare-ups that may be mistaken for acne. Yeast infections on the skin can also cause itchy spots on the chest or back, which can be confused with acne.
Understanding the nuances of these conditions is crucial for accurate diagnosis and effective treatment. Therefore, if standard acne treatments are not yielding results, it may be advisable to consult a healthcare provider for a more comprehensive diagnosis, which could include microbiological and endocrinological tests.
Latest articles

Hormonal Acne Treatment with Topical Creams

Cystic Acne on the Back: Best Treatment Options
Top Supplements for Treating Cystic Acne
